- Blog
- Nodus access case 2
- Aragami 2 all armor sets
- Demonomicon book of demons
- Transloader services ltd
- Aweeraser 2
- Letterpress tray
- Trainz simulator 2 mac download
- Clover configurator generate serial number
- Manual switchup to rail
- Double lumen tube
- Starmancer roadmap
- Women graphic tees
- Electroweb tm
- Fairy godmother tycoon plus crack
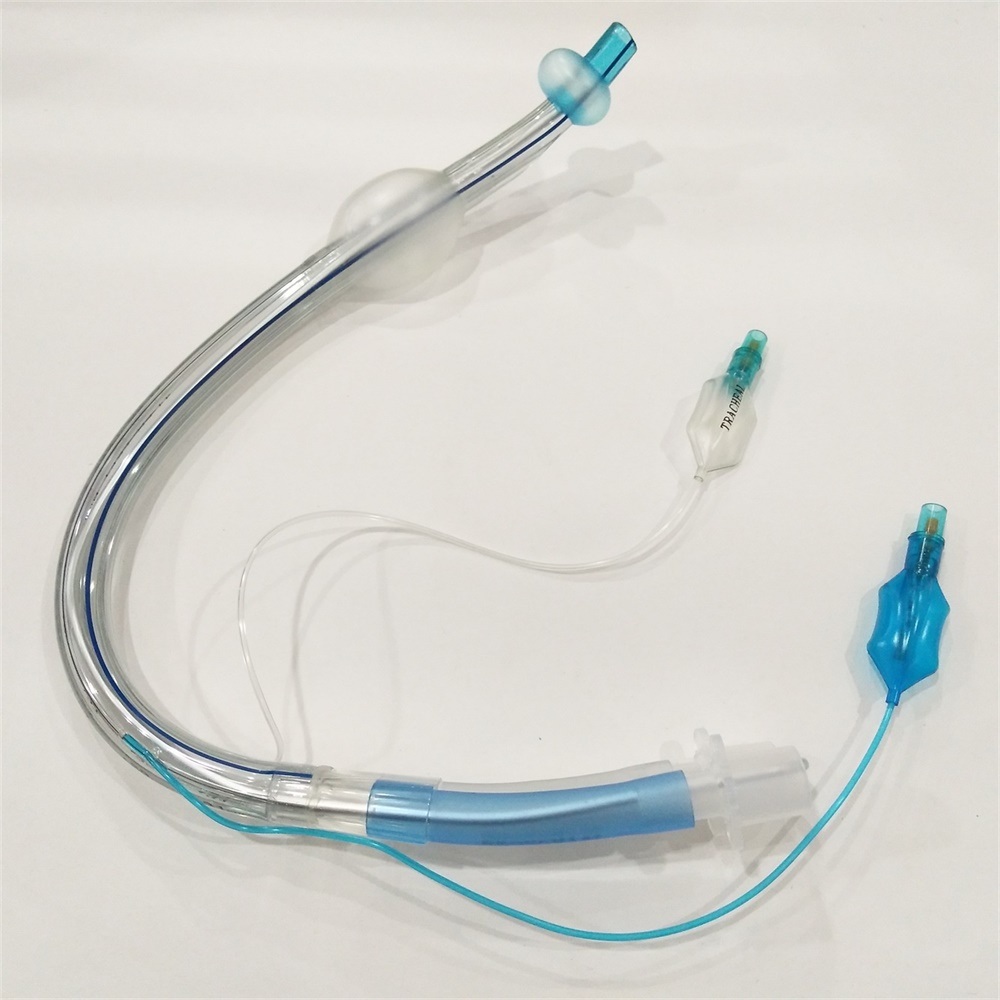

Air entry should be equal on both sides and there should be no leak around the tracheal cuff.
#DOUBLE LUMEN TUBE MANUAL#
Manual ventilation is commenced with the tracheal cuff inflated. The tube is then connected to the breathing circuit via a double catheter mount. As the tip is passed through the larynx, the tube is rotated 90 degrees to direct the endobronchial part to the intended side. The tube is held with the bronchial curve concave anteriorly (as with normal endotracheal tubes). Endobronchial blockers are a preferable choice for patients optimally managed with single-lumen endotracheal tubes rather than conventional double-lumen tubes. Ventilation to the pulmonary unit is blocked when the balloon is inflated. Endobronchial blockers are balloon-tipped catheters that are placed in the portion of the trachea that is to be blocked (usually the right or left main stem bronchus). An endobronchial blocker blocks ventilation to a pulmonary segment. Double-lumen endotracheal tubes isolate ventilation, separating the right and left pulmonary units using two separate endotracheal tubes. Double-lumen tubes and endobronchial blockers function differently. The decision to use an endobronchial blocker is clinical and should be based on a consideration of risk versus benefit. The indications for one-lung ventilation (OLV) are divided into two groups: absolute and relative. Thus, left-sided tubes are usually preferred, even for right-sided surgery, because of the risk of inadequate ventilation of the right upper lobe if incorrectly positioned. The main disadvantage of right sided tubes concerns the short length of the right main bronchus before giving off the upper lobe bronchus (risk of occlusion). They are passed blindly and their position should be confirmed bronchoscopically. The endobronchial parts are curved to the left or right. Double-lumen tubes all have cuffed endobronchial portions and tracheal cuffs. Endobronchial tubes are used in thoracic surgery.
- Blog
- Nodus access case 2
- Aragami 2 all armor sets
- Demonomicon book of demons
- Transloader services ltd
- Aweeraser 2
- Letterpress tray
- Trainz simulator 2 mac download
- Clover configurator generate serial number
- Manual switchup to rail
- Double lumen tube
- Starmancer roadmap
- Women graphic tees
- Electroweb tm
- Fairy godmother tycoon plus crack
